For years, we’ve all taken aspirin, ibuprofen (Motrin and Advil) and naproxen (Aleve) to relieve the common aches and pains of living.
Called “non-steroidal anti-inflammatory drugs (NSAIDs),” these drugs are effective against things like headaches, back pain, joint pain and muscle pain. You’ll find them in most households across the country because they’re so easy to use and because they’ve been established as safe for most people.
During the past decade, though, some studies have suggested that we all take a second look at how many of these pills we’re taking and how often. One recent study published in March 2017 linked the use of these drugs to an increased risk of heart attacks.
“We found that all common NSAIDs shared a heightened risk of heart attack,” said lead study author Dr. Michele Bally. “People minimize the risks because drugs are over-the-counter, and they don’t read labels. Why not consider all treatment options?”
Indeed, why not? To help you out, we gathered the top seven natural ways to ease chronic pain. If you find that you’re reaching for the aspirin a bit more often than you’d like, try these other options instead. There’s no reason why an alternative treatment may not work just as well or better for you.
Risks Associated With Common Pain Relievers
The link between pain relievers and heart attack is especially concerning because heart disease is already the leading cause of death for both men and women. The Centers for Disease Control and Prevention (CDC) states that about 610,000 people die of heart disease in the United States every year, which comes out to about one in every four deaths.
It’s not only the U.S., however. The World Health Organization (WHO) states that cardiovascular disease is the leading cause of death worldwide. We don’t need to be adding to it by taking drugs that could increase our risk. Yet, when we take NSAIDs, we do just that.
Researchers examining data from the Danish Cardiac Registry reported this year (2017) that all NSAIDs could increase the risk of heart attack by 31 percent.
“Allowing these drugs to be purchased without a prescription and without any advice or restrictions sends a message to the public that they must be safe,” study author Gunnar H. Gislason stated in a press release. “The findings are a stark reminder that NSAIDs are not harmless.”
He went on to warn that patients with cardiovascular disease or who have many cardiovascular risk factors should probably avoid using these drugs.
Other studies have shown similar links between NSAIDs and cardiovascular disease. The drugs are associated with other serious side effects as well. These include stomach bleeding, stomach ulcers and kidney failure.
These effects are particularly worrisome in older adults. Researchers reported in 2007 that seniors commonly take NSAIDs on a regular basis, and that chronic use increases the risk of peptic ulcer disease, acute renal failure, stroke, and heart attack. Given these concerns, it’s crucial to explore natural ways to ease chronic pain that do not carry such risks.
Many People Suffering From Chronic Pain Need Solutions
Despite these studies, NSAIDs are still considered generally safe as long as you use them only occasionally and at the recommended doses. However, there’s no doubt that there are many occasions in life when just an aspirin or two doesn’t do the trick.
Chronic pain affects about 50 million Americans, according to the National Institutes of Health. They add that “pain affects more Americans than diabetes, heart disease and cancer combined. It is a leading cause of disability, and it is a major contributor to health care costs.”
Chronic pain is defined as pain that lasts longer than a couple of days, persisting for weeks, months or years. It may be caused by a number of things, including injury, infection or a disease like arthritis or cancer. Other common types of pain like headaches, back pain and nerve pain also qualify as chronic pain.
This type of pain interferes with daily life, making it more difficult to work, play and spend time with loved ones. Without treatment, it can lead to depression and anxiety.
Finding relief is critical for health and well-being. So, if you’ve reached your limit on NSAIDs, what can you use instead? Explore these natural ways to ease chronic pain for effective alternatives to traditional pain relievers.
7 Top All-natural Options for Relieving Pain
Fortunately, there are many other natural ways to ease chronic pain that you can try. Below are seven options that have significant research behind them, making them more likely to work for you.
1. Pain-relieving Foods
Many common, everyday foods have been shown to help relieve pain. Tart cherry juice, for example, is frequently used by athletes and those with arthritis to tame inflammation, which helps soothe pain.
In a 2010 study, for example, healthy runners who drank tart cherry juice twice daily for seven days prior to running a long-distance race experienced a smaller increase in pain after the race than those who drank a placebo juice. Other studies have found that cherry juice and cherry pills, which contain flavonoids from cherries, may improve the stiffness associated with osteoarthritis. Recommended intakes are 16 to 24 ounces of tart cherry juice blend, one ounce of liquid concentrate or 400 milligrams of concentrate in tablets or capsules.
There are many other foods and beverages linked to pain relief. These include fatty fish and other foods high in omega-3 fatty acids, beet juice and pineapples. Find more in our post, “The 12 Best Foods to Ease Inflammation and Joint Pain.”

2. Herbs
Many herbs contain powerful components that help relieve inflammation and soothe pain. Ginger is a good example. It’s long been used as a natural pain remedy and has been found in modern studies to help ease joint pain.
In a 2012 study, researchers reported that ginger extract was just as effective in relieving osteoarthritis pain as medications like ibuprofen and cortisone. The key is to take a ginger supplement daily and give it time to buildup in your system. Then, see if you don’t notice a difference.
Other herbs that have shown in studies to help relieve pain include:
- Turmeric: You can use this together with ginger
- Feverfew: Found particularly useful in easing the pain of migraine headaches
- Basil: Helpful for joint swelling
- Capsaicin: Often used in topical pain-relieving creams
- Devil’s claw: Good for joint and muscle pain
- White willow bark: Contains the same component as aspirin
- Cinnamon: Recommended for easing muscle pain
- Boswellia: Can be used internally or topically
If you have joint pain, check out our article about the best natural joint supplements here.

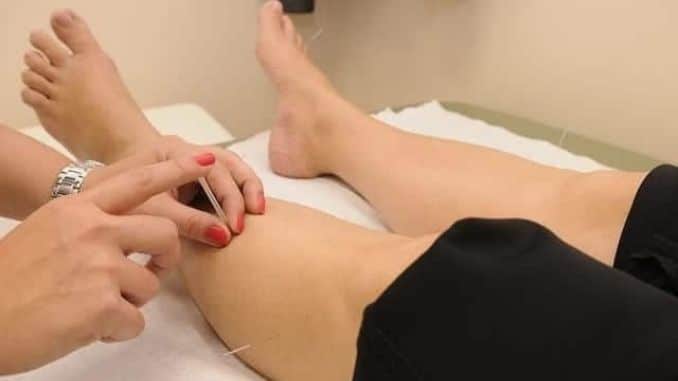
3. Acupuncture
If you haven’t tried acupuncture yet for natural ways to ease chronic pain, make an appointment today. This ancient Chinese practice has been associated with easing all sorts of pain, from migraines to arthritis to cancer-related pain.
One of the most recent and rigorous studies on acupuncture was published in 2012, and it provided strong evidence that acupuncture was effective for people suffering from osteoarthritis, migraines and chronic back, neck and shoulder pain.
Scientists analyzed 29 studies with a total of 17,922 patients and concluded that patients receiving acupuncture had less pain overall than those receiving sham treatments. “We think there’s firm evidence supporting acupuncture for the treatment of chronic pain,” said lead study author Andrew J. Vickers.
The treatment is equally effective for both adults and children, with government estimates showing that about 150,000 children in the U.S. underwent acupuncture in 2007.
4. Hydrotherapy (Water Therapy) for Natural Ways to Ease Chronic Pain
Water therapy or hydrotherapy is the practice of performing a series of exercises while immersed in water, such as in a pool or hot tub. Exercise is a pain-relieving activity to begin with, because it releases endorphins into the bloodstream, and endorphins are the body’s own natural pain relievers. In fact, they work in the same way that opioid pain medications work, by blocking receptors in your brain that typically receive pain messages.
So, exercise is good, but if you’re already in pain, you may find it difficult to move enough to get the blood pumping and the endorphins flowing. That’s where water therapy can help. The water helps support your body and provides a gentle resistance that gives you a real workout without taxing your joints or exacerbating joint pain.
Research has shown the benefits of hydrotherapy. In one study review published in 2014, researchers reported that it helped ease muscle soreness and muscle damage from exercise, eased the pain of fibromyalgia, soothed shoulder and knee pain and improved pain associated with rheumatoid arthritis.
5. Massage
You know that a massage can help you feel relaxed and refreshed, but studies have also shown that it can significantly reduce all sorts of pain. In 2017, scientists reported that regular massage therapy helped ease chronic lower back pain.
In an earlier 2010 study, researchers gave massage therapy to patients at the Flagstaff Medical Center in Flagstaff, Arizona. They found that patients receiving the massage reported lower levels of pain after their treatments than those who didn’t receive massage. They also reported increased relaxation and were able to sleep better.
Other studies have shown that massage therapy can help ease knee pain after surgery, soothe fibromyalgia pain, tame wrist pain and more. It works by increasing serotonin, the “good mood” neurotransmitter in the brain.
6. Mindfulness Meditation
It may be difficult to imagine that meditation or simply “being in the moment” could help reduce pain sensations, but research shows that it can.
This doesn’t mean that your pain is “all in your head,”. But on the other hand, there is a mental component to any experience of pain. It’s not only the actual pain that causes you discomfort—it is your brain’s interpretation of the pain. NSAIDs block pain receptors in the brain, so they don’t stop the pain ― they stop you from feeling it.
The Pain-Alleviating Power of Mindfulness Meditation
Researchers have found that mindfulness meditation can do the same thing. In a 2012 study, they acknowledged that increases in pain are usually associated with increased activity in certain regions of the brain. We can decrease the activity in these areas through meditation and also by focusing our attention on something else. It’s not always easy to focus when we’re in pain, however, and that’s why meditation can help.
Meditation requires that we focus the mind on one thing, such as a sound (“om”) or a sight (a candle flame) and allow all other thoughts to come and go without reacting to them. As we practice and get better at maintaining our focus without letting it wander. We get better at directing our thoughts.
Studies have shown that devout meditators from Nepal. For example, had a higher pain tolerance and lower subjective pain reports when compared to others their age. Chronic pain patients who completed an eight-week mindfulness program were found to improve their pain symptoms and overall quality of life. Mindfulness training was also shown to improve lower back pain and fibromyalgia pain.
In a 2016 study, researchers found that meditation, after a short training period. Reduced experimentally induced pain in a unique way and could be used in conjunction with other traditional pain relievers to enhance pain relief without additional side effects.
7. Yoga: A Holistic Approach to Natural Ways to Ease Chronic Pain
If you, like so many others, suffer from chronic low-back pain, you owe it to yourself to try yoga as it may help you to use fewer pain-relieving pills. This ancient form of exercise and stretching has been studied extensively for its pain-relieving capabilities and found to shine when it comes to the spine.
This is good news because back pain is typically stubborn and resistant to many other types of pain relief. Researchers from Boston Medical Center created a yoga class designed specifically for those suffering from back pain. It consisted of gentle poses like cat-cow, triangle pose and child’s pose. They then had patients with chronic back pain go through the class every week for three months. Then continue with more yoga sessions and at-home practice for nine more months.
Yoga: A Holistic Approach to Pain Management
At the end of the study, participants in the yoga classes were less likely to use pain medications after three months, because the yoga was effective at easing their pain—just as effective as physical therapy.
Harvard Health also notes that yoga can help people with arthritis, fibromyalgia, migraines and other types of chronic pain conditions. They point to one meta-analysis of 17 studies that showed yoga improved daily function in people with osteoporosis-related curvature of the spine.
The good thing about yoga is that it attacks pain in a number of ways, providing whole-body relief. The poses can help ease muscle and joint pain. While the meditative-like breathing calms the mind, reducing anxiety and stress related to pain.
“Yoga eventually influences all aspects of the person: vital, mental, emotional, intellectual and spiritual,” the researchers wrote. “It offers various levels and approaches to relax, energize, remodel and strengthen body and psyche.” It helps improve sleep and provides a moving sort of meditation that can help block the sensations of pain.
If you are looking for ways on how to bring back your natural vitality while relieving chronic inflammation and boosting up the natural fat burning hormones of your body, then check out the Best Foods that Rapidly Slim & Heal in 7 Days, here!