Brett had been running all his life but more intensely the past four years. He’d conquered a couple of marathons and didn’t plan to slow down anytime soon, but then he started to experience something new. After running for about five miles, his right knee would act up. Brett described it as “seizing up” as it became stiff and painful. It got harder to bend the knee, and after he finished his run, the soreness lasted for hours.
Brett stretched and iced and tried to run through it, but the pain only got worse. Soon, he couldn’t rest with his leg straight and bending his knee was extremely painful. Stairs became a huge challenge. He tried resting it again, but although he felt some better after about a week when he tried to return to running, the pain returned.
Brett was frustrated. This injury was interfering with his training schedule. So, he turned to his doctor and found out he had “Patellofemoral Pain Syndrome,” or “runner’s knee,” as it’s sometimes called. His doctor referred him to a sports exercise therapist, and Brett learned that for him, rest wasn’t going to be enough. He was going to have to strengthen and condition the affected area.
But how?
The Facts About Patellofemoral Pain Syndrome
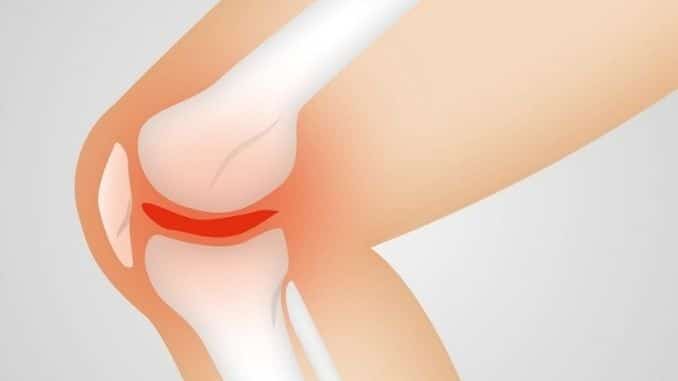
Patellofemoral pain syndrome (PFPS) is a term used to describe the pain that can occur in front of the knee and around the patella or kneecap. It may be called “runner’s knee” or “jumper’s knee” as it’s most common in athletes, although it can affect anyone at any time.
The syndrome occurs when something goes wrong in the tissues, tendons, and bone around the kneecap. Often, there is inflammation in this area, which causes the nerves to send out pain signals. To understand what’s going on, it helps to review the anatomy of the knee.
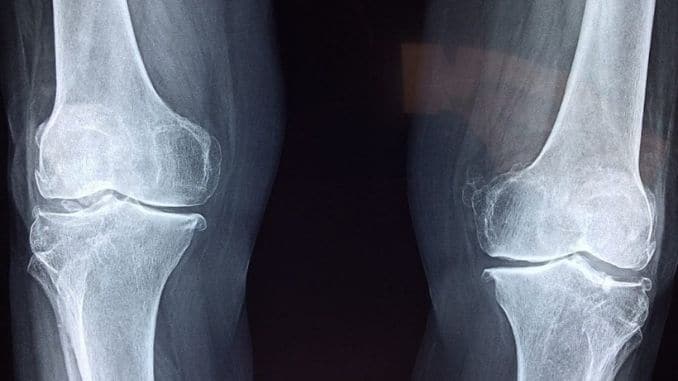
To form the knee, the thighbone (femur) comes down to join the shinbone (tibia), and the knee joint connects the two. Ligaments and tendons do the job of linking the bones together like ropes strung between the thigh and shin. The patella is the kneecap or top of the knee joint and is connected to tendons in the thigh and shin that help stabilize it.
At the top of the femur sits a groove called the “trochlea.” When you bend or straighten the leg, the patella moves inside this groove. The movement is usually smooth because of cartilage that covers both the groove and the end of the femur as well as the underside of the patella. Synovium fluid inside the knee joint also keeps things lubricated, so they move easily.
PFPS is the most common cause of knee pain in the United States. Researchers note that it constitutes 16 to 25 percent of all injuries in runners. They also state that forces on the patella range from between one-third and one-half of a person’s body weight during walking to three times body weight during stair climbing and up to seven times body weight during squatting. If the movement is off-center or uneven somehow, or if something is going wrong and straining the structures around the knee, pain may develop.
What Causes of Patellofemoral Pain Syndrome?
The most common cause of this syndrome is overuse. That’s why athletes often struggle with it. Vigorous physical exercises like running, climbing stairs, squatting, and participating in sports like basketball, tennis, or others that repeatedly increase forces on the knee, can all lead to PFPS. Suddenly increasing intensity in workouts like running for longer distances or playing twice a week instead of one can also result in pain.
The condition is more likely when a person’s anatomy or way of moving puts additional stress on the patella. Muscles, tendons, and the knee joint itself are all involved in what is called “patellar tracking” — how the patella moves inside the trochlea groove. If there are imbalances in the muscles, the knee joint becomes unstable, and the distribution of forces changes.
Abnormalities in patellar tracking are often at the root of PFPS syndrome. If the patella isn’t sliding as it should inside the trochlea groove, forces increase between the back of the patella and the trochlea, irritating the soft tissues and causing inflammation and pain. Why might the tracking be off?
- Hips and ankles aren’t aligned: If the hips and ankles are out of alignment during movement, the kneecap may shift too far outside or inside, increasing strain. This type of movement can also cause the patella to ride “too high” in the groove, again causing strain and inflammation.
- Muscles are weak or imbalanced: Strong muscles around the knee joint help to keep it stabilized and tracking correctly. If these muscles are weak or if some are strong and some are weak (an imbalance), the forces may be thrown off. Weak quadriceps in the thighs, for example, can cause poor patellar tracking.
There are some risk factors that can increase the risk of PFPS, as well. These include:
- Anatomic anomalies, which are things you were born with that you can’t change like knees that turn out and pronating feet
- Patellar hypermobility, which is when the patella moves more than normal
- Previous injury or surgery to the knee
- Tight tendons or muscles around the knee
- Training errors — overworking or underworking certain muscles
- Gender — women are twice as likely as men to develop PFPS — perhaps because a woman’s pelvis is wider, which increases the angle at which bones in the knee joint meet
- Having flat feet — increases stress on the knee joint
- Excessively worn shoes or shoes that don’t fit right
A small subset of patients may have what is called “chondromalacia patella,” which causes a softening and breakdown of the articular cartilage on the underside of the kneecap. As this cartilage is worn away, inflammation may result, causing pain.
What Does Patellofemoral Pain Syndrome Feel Like?
Pain is usually the first symptom of PFPS. Most describe it as a dull and aching feeling that occurs in the front of the knee. It tends to come on slowly while you’re doing your activities and then gets worse over time. Other common symptoms include:
- Pain behind, underneath, or around the kneecap
- A feeling of the knee “giving way”
- Pain when bending the knee, such as when climbing or descending stairs or squatting
- Pain after sitting for a long time
- Pain-related to changes in activity levels, equipment, or playing surfaces
- Popping or cracking sounds in the knee
- Stiffness in the knee joint.
Typically, the pain doesn’t go away — it sticks around, and even if it lessens during rest, it’s likely to come back during activity.
Diagnosing Patellofemoral Pain Syndrome
Rest is the first step in healing your PFPS. Give the knee a few days to heal. Try some ice packs and a knee wrap to help speed healing. Over-the-counter pain relievers can also help relieve swelling and pain.
After a few days of rest, don’t go straight back to the activities you were doing before. That likely cause the pain to return. Instead, find out what caused the pain in the first place. A doctor or physical therapist can help. He or she will likely have you perform a single leg squat and stand, if you can, to check for imbalances as you bend. He or she may also have you sit down and extend your leg out straight while watching your kneecap to see how it moves.
In another test, doctors may grasp the patella and move it from side to side to see how far it goes. This can help them tell if you may be too tight in some tendons and muscles or if the patella moves too much.
Once the doctor makes a diagnosis, you should have the information you need to determine what sorts of exercises and stretches will work best for you.
Exercises to Help Relieve Pain in Runner’s Knee
Moreover, a number of studies have shown that physical therapy is effective in treating PFPS. In one, researchers found that restoring good quadriceps strength and function was important to good recovery. Also. in another, they found that physiotherapy treatment provided a consistent improvement in short-term pain and function.
In 2002, researchers reported that patients who went through physical therapy for PFPS demonstrated a significantly greater reduction in scores for average pain and disability than did a placebo group who didn’t go through the therapy. Their program consisted of six treatment sessions, once weekly, and included quadriceps muscle retraining, patellar taping, and daily home exercises.
Furthermore, it’s best to talk to your physical therapist to determine which exercises are best for you, as each person has different reasons for developing PFPS. However, there are some standard exercises that may also help:
- Straight leg lift: Lie down on the floor. Bend one leg at a 90-degree angle with your foot flat. Tighten your quadriceps in the straightened leg and raise it up to a 45-degree angle. Hold for a couple of seconds, and then slowly lower down. Repeat 20 times, and then switch legs. Perform two or three sets per day.
- External hip rotation: Lie on your side with your knees bent at a 90-degree angle and “stacked” together. While keeping your heels together and your pelvis to the ground, lift your top knee as high as you can, hold for a couple of seconds, and then slowly lower down. Repeat 10 to 15 times per side for two-to-three sets.
- Wall slide: Stand with your heels about 6 inches away from a wall, and your feet about a foot apart. Press your back and buttocks against the wall. Slide your hips down the wall slowly until your knees are bent at a 45-degree angle. Hold for five seconds, and then slowly slide back up. Repeat 10 to 15 times for two or three sets.
If your muscles are tight, it’s also helpful to stretch them out. Moreover, ty these exercises:
- Hamstring stretch: Lie flat on your back and bend one knee toward you. Grasp the back of your thigh and hold. Then, straighten the leg in the air slowly until you feel the stretch in the hamstring. Hold for 5 to 10 seconds, lower down, and repeat with the other leg. Do 5 to 10 sets on each leg.
- Calf stretch: Stand facing a wall, about two feet away. Place your hands flat against the wall, and then step forward with one foot, bending the knee slightly. Moreover, lean your hips toward the wall, keeping both heels flat on the floor. Keep the back leg straight. You should feel a stretch in that calf. Hold for 20 seconds, and repeat three times. Do the same with the other leg.
- Side leg and buttock stretch: Sit down on the floor with one leg bent at a 90-degree angle and the other leg straight out. Twist your trunk to the right and use your arm to push against your bent leg. Feel the stretch in the outer leg and buttock. Hold for 20 seconds and repeat 5 to 10 times. Do the same with the other leg.
How Do I Prevent Patellofemoral Pain Syndrome?
You can also take steps to help you avoid this injury. Try these tips:
- Maintain a healthy weight: The more weight you’re carrying, the more stress on your knees. Losing even a few pounds can make a big difference.
- Warm-up and stretch: Start your workout with about five minutes of a light warm-up and stretch so your muscles don’t start out tight. Moreover, tight muscles can put extra pressure on the patella.
- Always increase activity gradually: If you want to run farther or step up your basketball game, always make your increases gradual. Sudden changes in intensity or duration can create stress on the knee that it’s not ready for.
- Get good shoes: Make sure you wear quality shoes that fit well and provide the shock absorption you need for the activity you’re involved in. Check with your podiatrist about any orthotics that may help with body alignment.
- Exercise weak areas: You want to keep the knee aligned properly as much as possible, so check with your physical therapist about exercises you can do to optimize strength in your legs and keep the patellar tracking normally.
- Put less pressure on the knee: Moreover, try exercises that put less pressure on your knee like swimming, anti-gravity treadmills, and biking. Ease yourself slowly back into your routine.
If you are looking for a fast, simple, safe, and effective program to eliminate your stubborn knee pain and patellofemoral pain syndrome, then check out the Patellofemoral Syndrome Solution program, here!