The Achilles tendon is the largest, thickest, and strongest tendon in the body but is prone to injuries, making Achilles tendonitis exercises essential for recovery and prevention.
The Achilles tendon is important [2] for movement but injuries, especially tears, can make it hard to move. A tear (partial or full) usually happens from a sudden or traumatic injury, causing pain, swelling, and then trouble walking.
Strengthening and stretching your Achilles tendon can boost flexibility, reduce stiffness, and then prevent injuries, helping you move better and stay pain-free.
Achilles Tendon Exercises
1. Standing Calf Stretch

For this exercise, utilize the wall for support if needed.
- Begin in an upright standing position facing the wall, with your feet hip-width apart.
- Maintain good alignment with your head, shoulder, hips, and then legs.
- Place both hands on the wall for Achilles tendonitis exercises.
- Engage your core and step a back with your one foot.
- Bend the front knee and lean towards the wall, feeling the stretch in the back leg.
- Hold this position for several deep belly breaths, in through your nose and then out through your mouth.
- Repeat the movement on the opposite side.
2. Seated Calf Stretch

For this exercise, utilize a towel, belt or resistance band.
- Begin in an upright sitting position on the floor with your legs extended and then closed together.
- Maintain good alignment with your head, shoulder, and then hips.
- After that, tighten your core.
- Loop the towel, belt, or resistance band around the ball of your feet and gently pull it towards you while keeping your spine and knees straight.
- Hold the position for several deep belly breaths, in through your nose and out through your mouth.
- Relax and then repeat the movement with 5 repetitions.
3. Seated Heel Raises

- Begin in an upright sitting position on a chair with your knees bent and feet flat on the floor, maintaining good alignment with your head, shoulders, and then hips.
- Place your arms on your lap.
- After that, engage your core.
- Raise your heel off the floor and then your toes on the floor for support.
- Hold this position for several deep belly breaths, in through your nose and then out through your mouth.
- Relax and repeat the movement with 5 repetitions.
4. Bent Knee Calf Raises

For this exercise, you can utilize the wall or the back of the chair for support if needed, and then a plyometric box or small step.
- Begin in an upright standing position in front of the chair and plyometric box, with your feet hip-width apart, maintaining good alignment in your upper body.
- Then, place both hands on the back of the chair for support.
- Engage your core.
- Step on the box or a small step and stand on it with your knees slightly bent, and then tuck your toes on both feet to lift your heels.
- Hold your movement for a couple of seconds.
- Lower your heels back down to the starting position and then repeat the movement.
5. Ankle Circles
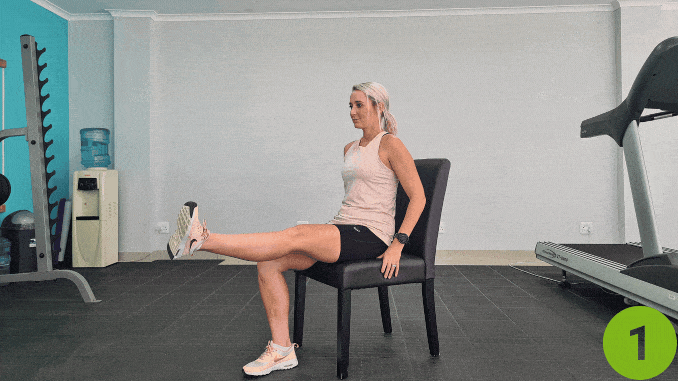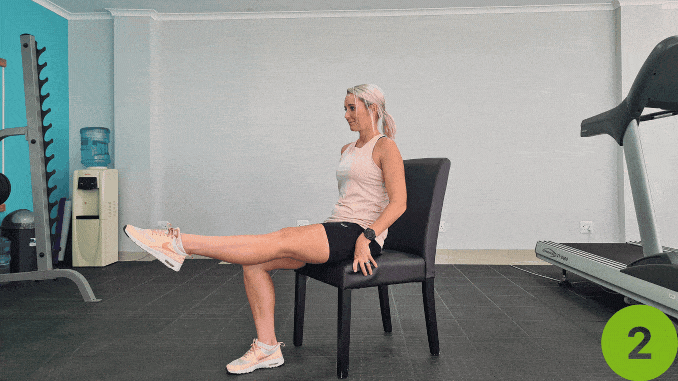
Doing achilles [3] tendonitis exercises early can help you recover and then gain the necessary range of motion.
- Begin in an upright sitting position on a chair with your knees bent and feet flat on the floor.
- Maintain good alignment with your head, shoulders, and then hips.
- Place your hands on your side.
- And then engage your muscles.
- Lift and then extend one leg in front of you while keeping your other leg bent.
- Rotate the ankle of your extended leg in a circular motion with 12 repetitions.
- Lower your leg down and then repeat the movement on the opposite leg.
Heel to Heal: Unlocking Recovery with Achilles Tendonitis Exercises
1. Single Leg Calf Raise

For this achilles tendonitis exercises , use a wall or anything stable and then sturdy for support and balance if needed.
- Begin in an upright standing position , maintaining a good alignment with your head, shoulders, hips, and then legs.
- Place your hands on your hips.
- Engage your core and then raise to your toes on both feet.
- Shift your weight onto your good leg and bend your knee to the affected leg.
- Lower your heel back down, following with the affected leg to return to the starting position.
- And then, repeat the movement.
- Complete the movement for 5-10 repetitions.
2. Single Leg Standing Balance

For this exercise , use the wall or the back of a chair for support and then balance if needed
- Begin in an upright standing position , maintaining a good alignment with your head, shoulders, hips, and then legs.
- Engage your core and then activate your glute.
- Shift your weight onto your good leg and bend your affected knee, while simultaneously keeping your balance on the supporting leg.
- Hold this position for several deep belly breaths, in through your nose and then out through your mouth.
- Lower your affected foot to return to the starting position.
- Basically, complete this movement for 2-5 repetitions.
3. Calf Rolls

- Begin in an upright sitting position with your knees bent and then feet flat on the floor.
- Engage your core and place your hands at your sides for support.
- Extend the affected leg out and in forehead and then place the massage ball under your calf area.
- Push from your hands to slightly lift your seat from the floor, then run the ball from the top to the bottom of your calf area and then back.
- Repeat the movement and for 2 sets of 10-15 repetitions.
If your arms lack strength, lean your back against the wall for support.
7 Specific Exercises and Stretches That Help Achilles Tendonitis
1. Ankle eversion

- Place the foot inside the loop of the band, then anchor the band to a stable object nearby.
- Using your ankle only (not the leg), pull the foot against the resistance band and away from the anchor object by moving your foot outward.
- Keep the knee straight.
- Repeat with each foot.
2. Ankle inversion
- Repeat the exercise above but pull the ankle in the opposite direction — inward instead of outward.
3. Ankle dorsiflexion
- Sit on a chair or exercise ball. Loop the band around your foot, then step on the ends of the band with the opposite foot.
- Using your ankle only in small movements, move your foot upward, toward your body.
- You should feel the work in your shin muscles.
4. Straight-Knee Heel Drop
- Stand on one foot on a step with the heel raised up and then over the space beneath.
- Lower the heel down gradually to be parallel to the ground.
- Keep the leg straight.
- Then, push up to the starting position and then repeat 3 to 15 times twice a day.
- If you’re already injured, when performing the exercise on your injured leg, use the good leg to help lift you back up, and then use the injured leg to lower yourself back down only.
- The exercise may be uncomfortable, which is ok. If it hurts a lot, talk to your doctor.
5. Bent-knee heel drop
- Again, stand on the step but, this time, bend your leg that you’re working at the knee.
- Raise the heel, and then slowly lower it to be parallel to the ground while keeping the knee bent.
- Return to the starting position and repeat 3 to 15 times twice a day.
- Follow the same instructions as those above if you are already injuired.
6. Wall Stretch

- Lean against a wall, both hands on the wall.
- Place one foot behind you with the leg straight and the heel on the ground, the other foot in front of it, knee bent.
- Push your hips toward the wall until you feel the stretch in your calf.
- Hold for 10 to 20 seconds, release and then repeat.
7. Bent-over stretch
- Stand with one foot in front of the other.
- Bend the back knee, and then bend forward over the other leg while keeping it straight.
- Grab onto the front foot underneath the toes and pull up on the toes until you feel a stretch in your calf.
- Hold for 10 to 20 seconds and then repeat on both sides.
Achilles Tendon Inquiries
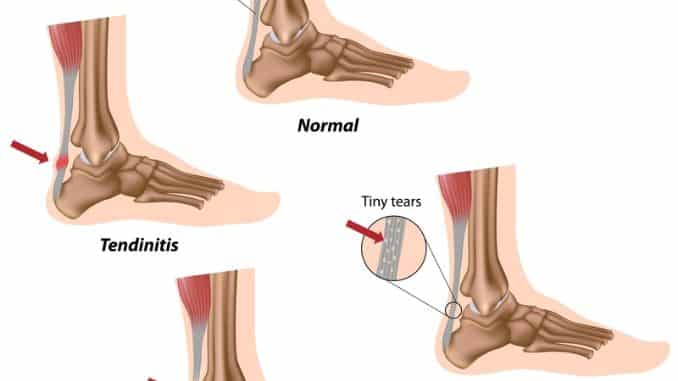
1. Achilles Tendonitis
- Inflammation of the tendon due to overuse, also known as Achilles tendonitis, can be managed with specific exercises.
- Common in runners and then people who suddenly increase activity levels.
- Symptoms: pain, stiffness, and swelling near the heel
2. Achilles Tendon Rapture
- Partial or complete tear of the tendon.
- Often occurs during explosive movements like jumping or sprinting.
- Symptoms: sudden sharp pain, a “popping” sound, and difficulty walking or pushing off the foot.
3. Achilles Bursitis
- Inflammation of the bursae (fluid-filled sacs) near the tendon.
- Caused by repetitive strain or improper footwear.
- Symptoms: swelling, tenderness, and pain at the back of the heel
What is the Strength of the Achilles tendon?
What do the figures say? How strong is the Achilles tendon? The Strength of tendons is related to their thickness and collagen content.
Tendons with more collagen type I fibers are more adept at withstanding larger loads.
What Causes Achilles Tendinitis?
The root cause of Achilles tendinitis is currently unknown. Inadequate footwear or walking abnormalities, which are associated with the condition, may be caused by tendon aging or by excessive training (Dubin, 2005).
As a central starting point, an injury involving the Achilles tendon occurs when the force applied to the tendon exceeds its ability to withstand the load. It may happen in a single episode or, more frequently, over some time, such as repetitive microtrauma.
Certain activities and improper body mechanics may also weaken, tire, or tighten the supporting muscles in the lower extremity, such as the gastrocnemius, quadriceps, and hamstrings.
When they tire out, Trauma is most likely to occur. When the Strength of the calf muscles is maintained, the Achilles tendon sustains its ability to endure the load.
Your footwear may also increase the risk of Achilles tendinitis. Frequent wearing of high heels shortens the tendon and calf muscles, leading to Achilles tendinitis and high heel pain.
Symptoms of Achilles Tendonitis

1. Pain
Pain is a sign of Achilles tendon injury; you usually feel this pain at the back of your heel or a bit above it.
It can hurt more when you’re engaging in sports, engaging in achilles tendon stretches after resting for a while, like when you wake up in the morning.
2. Stiffness
Stiffness and tenderness in the morning are indicators that you have Achilles tendonitis, and then performing Achilles tendon exercises can help alleviate these symptoms.
However, it can improve as you move around but worsen with prolonged or intense exercise.
The stiffness can improve as you move around, but it might return if you rest. Achilles tendonitis exercises can help alleviate this stiffness.
3. Swelling
- If you have Achilles tendonitis , there might be some swelling around the sore area.
- This swelling can make it feel uncomfortable and tight, especially when performing Achilles Tendon Exercises.
- You might even see the swelling—a common sign that something is inflamed, which means it’s irritated or swolen.
4. Reduced Range of Motion
- Achilles tendonitis can limit the range of motion in the ankle and foot.
- People who are affected by it may find it challenging to flex their feet or point their toes fully.
- This reduced flexibility can contribute to difficulty with activities requiring a full range of ankle motion.
5. Tenderness
- Tenderness to the touch is another characteristic symptom.
- The Achilles tendon becomes sensitive, and pressure on the affected area may cause even more pain, making it difficult to lower your heels.
Overview of Treatment Options
1. Ice

Using ice on the affected area helps reduce inflammation and then alleviates pain.
Cold therapy can be administered through ice packs or ice baths while keeping the affected leg straight, shortening recovery.
However,it is typically recommended for short durations and should be wrapped in a cloth to prevent direct contact with the skin to avoid ice burns.
2. Rest
Rest is a vital aspect of Achilles tendonitis treatment, involving a deliberate reduction or temporary cessation of activities that place undue strain on the Achilles tendon.
This pause allows the injured tendon to recover and then reduce inflammation with Achilles Tendon Exercises.
Actions such as elevating the foot, keeping the knee straight, and performing Achilles Tendon Exercises.
In addition, recognizing the significance of rest and its impact on recovery is essential, and then inexperienced individuals should consult healthcare professionals for their next action.
3. Medication
Anti-inflammatory drugs like ibuprofen or naproxen are commonly recommended for Achilles tendonitis to reduce pain and then inflammation by lowering the levels of contributing chemicals.
Following recommended dosages is crucial, and then communication with healthcare professionals is key for effective pain management.
In more severe cases, stronger medications may be advised, along with Achilles tendonitis exercises.
However, it’s important to understand that medication is part of a broader treatment plan that includes rest, physical therapy, and lifestyle adjustments for optimal Achilles tendonitis symptom management.
4. Surgery
Surgical intervention might be considered for severe cases of Achilles tendon disorders where conservative measures fail.
Surgery may involve removing damaged tissue, repairing the tendon , or, in rare cases, a complete reconstruction.
Furthermore, this option is typically reserved for cases with a significant tear or degeneration of the tendon.
5. Exercise
Exercise plays a crucial role in Achilles tendonitis treatment.
However, focusing on specific exercises that promote recovery without causing further damage is essential.
Eccentric exercises , stretching, and then strengthening routines are commonly prescribed.
Physical therapy may be recommended to guide patients through a structured, comprehensive program.
Conclusion
Achilles tendonitis can be a challenging condition to overcome, but with the right exercises and rehabilitation techniques, it is possible to achieve relief and recovery.
Remember to start slowly and gradually increase the intensity and frequency of your exercises.
It’s also important to listen to your body and stop if you experience any severe pain or discomfort.
Struggling with Achilles Tendinitis? Don’t let pain slow you down! Start incorporating targeted exercises to strengthen your Achilles tendon, improve flexibility, and reduce discomfort.
Try our Achilles Tendinitis Exercise Solution today and take the first step toward recovery. Get back on your feet with safe, effective movements that promote healing!
FAQs
What is the best exercise for Achilles tendonitis?
The best exercise for Achilles tendonitis is the standing calf stretch. Stand facing a wall, place your hands on it, step one foot back, and bend the front knee. Hold the stretch, feeling it in the back leg and calf muscles. Repeat on both sides. This stretch helps improve flexibility and reduce stiffness in the Achilles tendon and calf muscles.
What is the fastest way to heal an Achilles tendon?
Healing speed can vary depending on the severity of the injury. A combination of rest, ice, compression, and elevation (R.I.C.E.) in the early stages, followed by physical therapy, can help. It’s crucial to avoid pushing through pain and follow a structured rehabilitation program.
Dr. Jared recommends staying away from activities that put stress on the tendon and using a mix of stretching, strengthening exercises, and self-care like icing and massage to help it heal.
What is the best exercise for a torn Achilles?
After a torn Achilles, exercises should focus on gentle movement and strengthening as healing allows. Early exercises might include gentle range-of-motion exercises and gradually progressing to eccentric strengthening exercises as you regain strength and mobility. Always seek guidance from a healthcare professional, especially post-surgery or during early recovery.
What strengthens the Achilles tendon?
Eccentric calf raises, heel drops, and resistance band exercises that target the calf muscles can help strengthen the Achilles tendon. Building strength in the calf muscles is important for reducing strain on the Achilles and improving its function. Consistency and gradual progression are key to safe and effective strengthening.


