The United States Department of Health and Human Services states that about one in 10 women of childbearing age is affected by polycystic ovary syndrome (PCOS). It used to be that doctors believed the condition was mainly one that affected fertility, but more recent research suggests it may have more serious long-term effects on a woman’s health.
Currently, there is no cure for PCOS — only treatments that help manage the symptoms. Scientists are hard at work trying to learn more, in the hopes of finding new ways to treat it and, eventually, prevent it from developing in the first place.
What Is PCOS?
Women with PCOS have an imbalance of reproductive hormones. Doctors don’t know what causes this imbalance, but they do know that the following hormones are most affected:
- Luteinizing hormone (LH): Together with the follicle-stimulating hormone (FSH), LH encourages the release of the egg from the ovary during the process of ovulation. Women with PCOS often have an LH level that is two to three times higher than the FSH level. This disrupts ovulation and can cause the ovaries to release too much testosterone.
- Androgens: These include testosterone and are also called “male hormones” because they are more prevalent in men and control the development of male traits and reproductive activity. All women make small amounts of them too, producing them in the ovaries where they help stimulate puberty and regulate other functions in the bones, kidneys, liver, and muscles. Women with PCOS make more androgens than normal, which can prevent the ovary from releasing an egg during the menstrual cycle and may cause excess hair growth, acne, and male pattern baldness.
- Insulin: This is the hormone that transports fuel ― in the form of the sugar, also known as glucose ― from foods eaten into the body’s cells where it can be used. Its action helps keep blood sugar levels stable. Levels of insulin tend to be high in many women with PCOS, which indicates the body is unable to use its insulin as well as it should and, therefore, has to produce more to keep blood glucose levels under control. Women with PCOS who are overweight are more likely to have trouble with insulin.
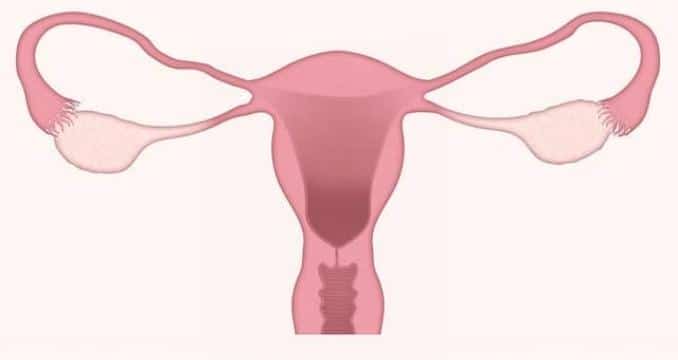
In addition to a hormonal imbalance, women with PCOS may also have cyst-like growths on their ovaries. Although not always present, the growths are common enough that if they exist along with a hormone imbalance, the two together are seen as clear signs of PCOS.
The name “polycystic ovary syndrome” indicates multiple cysts on the ovaries, but the term is a little misleading as the growths are partially formed follicles. Fortunately, they usually resolve on their own and, even if they remain, they are rarely harmful.
Follicles are small sacs filled with fluid that is normally found inside the ovaries. They secrete hormones that affect the menstrual cycle, and each one has the potential to release an egg for fertilization.
When everything goes right, one follicle becomes dominant, grows and develops the egg for fertilization, and then ruptures and releases that egg. The egg travels into the uterus and, if it’s not fertilized, it is flushed away during the bleeding cycle. Then, the process starts over again.
In women with PCOS, abnormal hormone levels prevent the follicles from growing and releasing their eggs as they should. Instead, these immature follicles accumulate in the ovaries, partially growing to resemble cysts (fluid-filled sacs). Because they don’t release eggs, they further disrupt hormone levels, causing estrogen and progesterone to drop and androgens to rise.
What Causes PCOS to Develop?
Scientists don’t know why some women get PCOS and others don’t, but they do have some theories. One is that the disorder runs in families, meaning that genetics may be a factor. Some studies have identified genes that seem to be linked to the condition.
Another theory is that insulin may be to blame. If the body’s cells become resistant to the insulin, similar to that which occurs in type 2 diabetes, blood sugar levels can increase, causing the body to produce more insulin. All that insulin can encourage the release of more androgens, disrupting ovulation.
A third theory is that inflammation may be involved. Research has found that women with PCOS typically have a chronic, low-level inflammation that stimulates the ovaries to produce more androgens.
Some newer studies also suggest that elevated hormones during the pregnancy could cause the infant to be born with a higher risk for PCOS. In one animal study, researchers found that levels of one hormone called “anti-Mullerian hormone (AMH)” was different in pregnant women with PCOS and those without the condition.
They found that the babies born to the mothers with PCOS were likely to show symptoms of PCOS themselves. Scientists also found that treatment to normalize this hormone was effective in not only preventing the disease from being passed on but easing symptoms in those subjects who already had it.
What scientists are starting to believe now is that it takes a combination of these and perhaps other factors for PCOS to develop. It’s probably not caused by just one thing. So far, however, there is still little clarity on exactly what factors may lead someone to develop the condition. The research is ongoing.
What Are the Symptoms of PCOS?
You may be having symptoms and wonder if PCOS is to blame. Below are the most common symptoms associated with the disorder. Keep in mind that some women may have most of these symptoms and others may have only one or two.
It’s also important to check with a doctor as PCOS is a complicated disorder and requires a complete medical examination for diagnosis. Doctors will typically ask questions about your menstrual cycle and take a blood test to check hormone levels and may also conduct an ultrasound test to view the reproductive organs:
- Irregular periods or no periods at all
- Heavy bleeding when bleeding finally occurs
- Headaches caused by unbalanced hormones
- Difficulty getting pregnant because the follicles aren’t releasing eggs as they should
- Excessive hair growth, often on the face, chest, back or buttocks
- Thinning hair or hair loss on the head
- Oily skin or acne
- Dark patches of skin on the back of the neck, under the arms or in the groin area and are caused by higher levels of insulin
- Weight gain or trouble losing weight
What About PCOS and Infertility?
If you are diagnosed with PCOS, that doesn’t mean you can’t have children. Some women can still get pregnant, but it is true that the disorder is one of the most common causes of infertility. Fortunately, it is treatable in most cases. Several medications are available to help restore ovulation in women who are struggling.
These medications stimulate the hormones needed to get the follicle to mature as it should and to release an egg. Injections of synthetic hormones can also help encourage the follicles to grow. If insulin is a problem, other medications can lower insulin and androgen levels, helping to stabilize the normal ovulation cycle.
Once a PCOS patient becomes pregnant, the problems aren’t necessarily over. PCOS can cause complications during pregnancy, including:
- Premature birth
- Miscarriage
- High blood pressure
- Gestational diabetes
- Ectopic pregnancy
Most women under a doctor’s supervision can carry a healthy baby to term. In a 2009 study, researchers found that among women who had attempted a pregnancy, 86.7 percent of PCOS patients and 91.6 percent of controls gave birth to at least one child. In other words, most women with PCOS were still able to carry to term.
In a later 2014 study, results showed that the number of children per woman was similar in both those with PCOS and those without, although the women with PCOS were more likely to have used infertility services. Researchers also noted that PCOS itself was not independently associated with pregnancy loss, but that other risk factors like a high body mass index (BMI) were.
Important steps to take to increase the odds of a successful pregnancy include:
- Managing blood sugar levels
- Avoiding too much weight gain
- Eating a healthy diet
- If you’re overweight, try to lose some weight before becoming pregnant
What Are the Long-term Effects of PCOS?
Unfortunately, PCOS affects the entire body, not just the reproductive system. Studies have found that it can increase the risk of other health problems, including:
- Type 2 diabetes
- Cardiovascular disease
- Stroke and heart attack
- Metabolic syndrome, which is a collection of factors including high blood sugar, high blood pressure and high blood cholesterol that contributes to diabetes and heart disease risk
- Endometrial hyperplasia, which can increase the risk of endometrial cancer
- Sleep apnea, particularly if the person is overweight
- Depression and anxiety
It’s important to be aware of these risks and to take steps to prevent them. A healthy lifestyle along with regular doctor checkups can keep PCOS from causing more serious problems as you get older.
How Is PCOS Treated?
Common conventional treatments for PCOS include:
- Birth control: In women who don’t want to become pregnant, birth control pills or patches or rings can help restore normal hormone balance, regulate ovulation and relieve symptoms as well as reduce the risk of endometrial cancer.
- Diabetes medications: For women with insulin resistance or who have been diagnosed with type 2 diabetes, medications can help control blood sugar levels.
- Hair removal treatments: For women with excess hair growth, there are treatments that can help slow it down. These are usually available in creams and ointments. Cosmetic procedures like laser hair removal and electrolysis can also remove unwanted hair.
- Fertility drugs: In women who want to get pregnant, there are medications available that can help encourage ovulation. They can sometimes increase the risk of multiple births.
- Surgery: This is the last resort treatment for women who haven’t had success with other fertility treatments. Doctors use a minimally invasive procedure to address thickened ovaries and help restore ovulation
In addition, there are lifestyle changes patients can make to help reduce symptoms. These include the following:
- Lose weight: If you’re overweight, losing even a little bit can help reduce symptoms as it can reduce insulin and androgen levels. Losing weight also helps reduce the risk of problems during pregnancy.
- Limit carbohydrates: Adopting an anti-diabetes diet can help keep blood sugar levels stable. Avoid carbohydrates and high-fat items and check the glycemic index for foods that break down more slowly in the body and keep blood sugar levels more even.
- Exercise regularly: This can help keep your body weight under control and also helps lower blood sugar levels.
- Get enough sleep: Some studies have indicated that women with PCOS may be more likely to have sleep problems because of an overproduction of the sleep hormone, melatonin. If you’re noticing problems, try to improve your nighttime routine so that you feel sleepy, and talk to your doctor about other options.
- Get enough vitamin D: Scientists have found that many women who have PCOS are deficient in vitamin D. Although they don’t believe the deficiency causes the syndrome, they do think that it can increase symptoms.
For your guide to the best foods to heal your body, check out The Best Foods that Rapidly Slim & Heal in 7 Days, here!