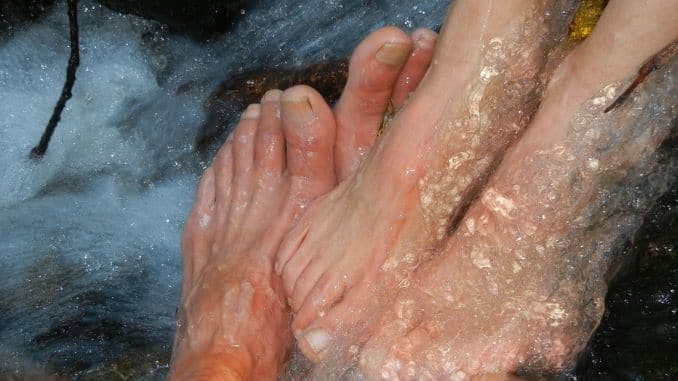
It’s not unusual for your fingers and toes to suffer during the winter season. There’s a reason those foot and hand warmers are such popular gifts over the holidays, say nothing of those thermal lined gloves and boots.
However, there are cold hands and feet, and then there are abnormally cold hands and feet, which are often caused by a condition called “Raynaud’s syndrome.” What is this condition, and how can you tell if you may be affected?
What Is Raynaud’s Syndrome?
Raynaud’s syndrome (or Raynaud’s disease or phenomenon) is a rare disorder that affects the blood vessels. It causes them to overreact to cold or stress and become severely narrowed or even shut down.
It’s normal for blood vessels to shrink a little in response to the cold. It’s the body’s way of redirecting blood to the central organs ― to protect them and ensure survival.
In those with Raynaud’s, however, the reaction is exaggerated to the point of potential injury. The blood vessels shrink suddenly in response to even small changes in temperature and remain so for too long, reducing blood flow to the skin and leaving fingers and toes without the proper circulation.
When this happens, blood pools in the constricted blood vessels and becomes oxygen-deprived, which is why the area may turn blue. Possible triggers include not only changes in temperature but also stress or emotional upset, dipping the hands in cold water, or taking something from the freezer. In time, the affected blood vessels may thicken, limiting blood flow further.
When warmth or calm returns, the blood vessels open up again, and the skin may flush, turn red, throb, or tingle. In some people, the fingers and toes hurt as they warm up.
Raynaud’s primarily affects blood vessels in the fingers and toes, but it can also affect those in the nose, lips, ears, and even nipples. After warming, it can take more than 15 minutes for the blood flow to return to normal in the affected areas.
Doctors typically separate Raynaud’s into two different types:
- Primary Raynaud’s: Develops on its own. The cause is unknown. It typically begins between the ages of 15 and 25 and is less severe than secondary Raynaud’s. Patients tend to describe it as more bothersome than disabling.
- Secondary Raynaud’s: Develops because of an injury, trauma, disease, or because of certain medications. The diseases most commonly associated with Raynaud’s include autoimmune diseases and connective tissue diseases like lupus, scleroderma, rheumatoid arthritis, Buerger’s disease, Sjögren’s syndrome, atherosclerosis (artery narrowing), thyroid disorders, pulmonary hypertension, and polymyositis. This type is usually more dangerous, occurs later in life and can damage blood vessels, and lead to problems with dexterity and ulcers, which are wounds in the hands and feet that resist healing.
Symptoms of Raynaud’s include:
- Cold fingers or toes in response to cold, stress, or emotional upset
- Color changes in the skin that occur in response to the cold or stress — skin turns pale or white at first, then possibly blue and then red upon warming
- A numb, prickly feeling
- Throbbing, tingling, and swelling upon warming
- Stinging pain upon warming or stress relief
- In severe cases, sores may form on the finger pads
What Causes Raynaud’s Syndrome?
Scientists don’t yet know what causes Raynaud’s syndrome. Much research has been done on the condition, but it’s still poorly understood. There are some theories. It could have something to do with the neurochemicals in the brain and how they react to changes in temperature. The blood vessels could be malfunctioning, producing too many constricting substances.
Some genes may also be to blame. Scientists have identified several that may be involved, and studies have shown that the condition tends to run in families. Because it develops more commonly in women of childbearing age, there is also some speculation that the female reproductive hormone estrogen may be involved.
The risk factors for Raynaud’s syndrome include:
- Being female — the condition is more common in women than in men
- Family history of the disease — about 30 percent of first-degree relatives of people with primary Raynaud’s also have the condition
- Having an autoimmune disease
- Having a connective tissue disease
- Cigarette smoking
- Having carpal tunnel syndrome
- Suffering an injury or trauma that affects the blood vessels like a wrist fracture, surgery, or frostbite
- Chemical exposure
- Having undergone chemotherapy treatment in the past
- Repetitive use of vibrating tools like a jackhammer
- Repetitive actions like typing or playing the piano for long periods
- Side effects of certain medications, including high blood pressure, migraine, attention-deficit/hyperactivity disorder, decongestant, and over-the-counter cold medications
How to Find Out if You May be Suffering From Raynaud’s Syndrome
Everyone suffers from cold fingers and toes now and then, so how can you tell the difference between a normal cold feeling and a more serious lack of circulation?
First, watch for a difference in symptoms. It’s normal to have cold hands and feet when it’s super cold out. If you notice a similar reaction when you feel stressed or emotionally upset, however, or when the temperatures aren’t that bad ― and others aren’t suffering similar symptoms ― you may want to see your doctor.
Second, check your skin for color changes. Cold fingers and toes may appear a little red, but Raynaud’s cold fingers and toes may look white or blue. If you notice these two colors, that’s a clear sign you may be suffering from this syndrome.
Finally, check with your doctor. Your physician will listen to your symptoms and look at your medical history to determine a diagnosis. A cold stimulation test may also be used to determine if the cold triggers your symptoms.
For this test, the doctor attaches a small thermometer to your fingers, then inserts them in ice water for a few moments before removing them. The thermometer records how long it takes your fingers to return to a normal temperature. A result of 15 minutes or less is considered normal, whereas more than that may indicate Raynaud’s.
If Raynaud’s is suspected, you may undergo another test called a “capillaroscopy” to see if it’s the primary or secondary type. During this test, the doctor puts a drop of oil on the skin at the base of the fingernail, then examines the finger under a magnifying lens for enlarged or malformed capillaries, which are a sign of secondary Raynaud’s.
If this test is positive, your doctor may perform other tests to pinpoint the condition that may be associated with the Raynaud’s.
10 Ways to Manage Raynaud’s Syndrome
In some cases, doctors may prescribe medications to help ease symptoms of Raynaud’s. These may include drugs that relax the blood vessels and open them up so the blood will flow more easily.
Otherwise, the best treatment is lifestyle changes that can help support healthy blood vessels and protect your fingers and toes from damage. In severe cases, surgery may be required to help heal the nerves or manage severe pain.
1. Avoid Your Triggers
Whether your symptoms arise because of cold temperatures, stress, or emotional upset, your best approach is to try to avoid these triggers. Stay warm and practice daily stress relief and mindfulness to keep your emotions even and centered.
2. Wear Warm Clothes
This is your excuse to splurge on quality gloves or mittens and liners, boots, socks and hand, and feet warmers. Wear a coat with snug cuffs or extended hand covers to prevent cold air from reaching your hands. Don’t forget a hat as keeping the entire body warm helps keep your hands and feet warm too.
Some people suffer an attack when in air-conditioned spaces. If this happens to you, keep a sweater or jacket with you to wear in these locations, and take your gloves along as well.
Take this seriously, as it’s about your health and your ability to continue to move your fingers and toes normally. Protect yourself as well as you can. If you need to wear heavy socks or gloves even when indoors, such as when you’re stressed, or when going to bed, don’t hesitate to do so.
3. Exercise Regularly
Exercise gets the heart beating and the blood flowing and can help keep your blood vessels healthy in time. Avoid exercising in the cold, however, and always take care to keep your fingers and toes warm.
4. Treat an Attack Immediately
If you notice the condition flaring up, don’t wait — take immediate action. The best approach is to get to a warm location and soak your hands and feet in warm, not hot, water. If this isn’t possible, wiggle your fingers and toes and try to get them somewhere else warm. You may put your fingers under your armpits, for example, or massage your feet.
5. Practice Regular Stress Relief
If stress triggers your attacks, adopt a routine of stress-relieving activities. These may include exercise, journaling, coloring, crafting, daily walks, deep breathing, tai chi, yoga, listening to calming music, meditation, and progressive muscle relaxation.
Making a habit out of stress relief is more likely to help than if you wait and use these methods only when feeling stressed. A regular daily stress-relieving activity can help train your system to relax more in general, which can help reduce your attacks.
6. Stop Smoking
Smoking cigarettes can cause the blood vessels in your body to constrict and damages them as well. If you smoke, do your best to quit.
7. Try Acupuncture
There is evidence that acupuncture can help facilitate blood flow, and some studies have found success with the treatment in patients with Raynaud’s.
In one study, patients with primary Raynaud’s were divided into two groups:
- Group 1 underwent seven acupuncture treatments during a two-week period.
- Group 2 served as a control group and received no treatment.
All patients kept a daily diary of their symptoms and attacks. Results showed the treated patients experienced a significant decrease in the frequency of attacks — by 63 percent overall compared to the control group.
8. Try Gingko Biloba
Gingko Biloba is an herbal supplement that has antiplatelet activities, meaning that it may help to support normal blood flow.
In a 2002 study, researchers studied this herb in patients with Raynaud’s disease. They gave one group a standardized Ginko Biloba extract and the other group received a placebo. At the end of the 10-week study period, those who received the ginkgo Biloba reported an average of a 56 percent reduction in the number of attacks per week, compared to a 27 percent reduction in the placebo group.
9. Take a Fish Oil Supplement
Fish oil supplements are high in essential fatty acids, which may help reduce symptoms in those with Raynaud’s, particularly primary Raynaud’s. In one small study, patients taking fish oil capsules daily were able to improve their tolerance to cold — they could be in the cold for longer periods before their symptoms developed. The researchers thought the effects were due to improvements in blood pressures in cold temperatures.
10. Avoid Caffeine and Alcohol
Both of these substances can trigger Raynaud’s attack in some people. Studies have shown that heavy alcohol use, in particular, is associated with an increased risk of Raynaud’s syndrome. Caffeine naturally constricts blood vessels, which is why it can help relieve a headache, but it can also make Raynaud’s worse.
For your guide to relieving tennis elbow pain, make sure to check out the Tennis Elbow Pain Solution, here!
.