Today, I have a guest blog post from Eric Cressey on what to do about loose joints.
Enjoy!
~ Rick
=====================
In this era of boot camps and semi-private training. Trainers must go out of their way to ensure that certain clients don’t get “lost in the shuffle.” Perhaps no plan is more important than dealing with clients with considerable joint hypermobility. Also known as “loose joints” or “joint laxity.”
At birth, we all have varying degrees of congenital laxity. Meaning some of us have less ligamentous “give” than others do. Just like someone might make more or less of a certain hormone, certain individuals are more efficient at synthesizing collagen. So they wind up with a lot more joint range-of-motion (ROM). People with congenital laxity aren’t super adept in this regard.
In certain situations, this can be beneficial; throwers, swimmers, and gymnasts can use this natural predisposition toward freaky ROM to be more successful in their sporting disciplines. However, it also predisposes these individuals to musculoskeletal issues, ranging from ankle sprains to shoulder subluxations, stress fractures, hernias, and early osteoarthritis.
Also, these folks are more likely to have detached retinas and gastrointestinal reflux disorder (and a host of other issues) because collagen deficiency affects not just skeletal muscles, tendons, and ligaments but also visceral organs (smooth muscle), skin, blood vessels, and the tissues of the eye.
Dr. Alan Pocinki on Hypermobility
Dr. Alan Pocinki, a renowned expert in this field, states, “To compensate for stretchy blood vessels and increased venous pooling (too much blood collecting in over-stretched veins). Most people with hypermobility appear to make extra adrenaline, which may account for high energy. Always-on-the-go lifestyles of many hypermobile people.” This is one reason why it’s not uncommon for hypermobile individuals to have anxiety issues and panic attacks. They are in a chronic sympathetic nervous system overload. This has implications in terms of poor sleep quality and impaired recovery capacity.
Further, Pocinki note, “Because too much blood is pooling instead of circulating. People with JHS [joint hypermobility syndrome] typically have cold hands and feet and low or low-normal blood pressure and lightheadedness on standing.”
3 Quick Tips
With all this in mind, we can appreciate that it’s imperative to identify the most hypermobile clients we have before starting their exercise programs. Here are three quick tips on this front:
1. Take note of age, ethnicity, and gender, age. Laxity becomes less prevalent as we age. You’ll see it more commonly in those of African, Asian, and Arab origin than in Caucasians. It’s also more common in females than males.
2. Note the “feel” of the handshake. You’ll typically feel a lot of “give” in these individuals’ handshakes, and their hands will often be cold even when it’s really warm in the environment. Their knuckles might even pop a bit.
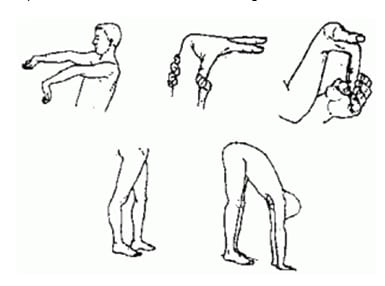
3. Do a Beighton Hypermobility Test. The screen consists of five tests. (four of which are unilateral), and is scored out of 9; a higher score is indicative of greater hypermobility:
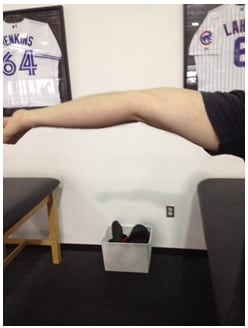
- Elbow hyperextension > 10° (left and right sides)
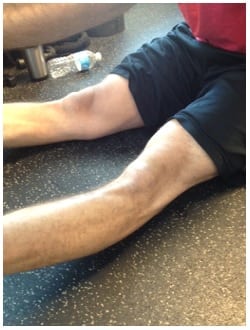
- Knee hyperextension > 10° (left and right sides)
- Flex the thumb to contact with the forearm (left and right sides)
- Extend the pinky to >90° angle with the rest of the hand (left and right sides)
- Place both palms flat on the floor without flexing the knees
EricCressey.com: Beighton Score – Assessing Hypermobility/Laxity
Now, considering a sedentary population, many trainers assume all individuals are incredibly tight and need to stretch until the cows come home. With that in mind, here’s a great example of an athlete who – at 6-4, 240 pounds – wouldn’t appear hypermobile to the naked eye. However, when you run a Beighton test, you quickly see that he’s got a lot of laxities, and his programs need to focus on building stability first and foremost.
Stretch him, and he’ll get worse. Build stability, and he’ll thrive – all because you ran some simple tests ahead of time.
So, we know that if we’ve got these hypermobile people under our care, we don’t want to be stretching them. What do we do when they always feel “tight?” And, they absolutely will say this is the case all the time.
They feel “tight” because their bodies will lay down trigger points to lay down stability where they otherwise lack it protectively. You destroy their joints and continue the painful cycle if you stretch them. Instead, these individuals need to work on building stability within the ROM they already have with quality strength training. For the trigger points, they can do some extra foam rolling or get massage work done, especially if it helps them to wind down and shut off the sympathetic nervous system (fight or flight) for a bit.
In terms of training them, most things are fair game, but you need to ensure that they aren’t exaggerating the ROM on exercises; they need to stop short of where their end range is. A great example is elbow hyperextension on push-ups; this is not something you want to see!
Final Word
Finally, monitor what they do between sets. A lot of hypermobile individuals will stretch while they’re resting without even thinking about it. We like to do what we’re good at, so you must go out of your way to coach these individuals out of those habits.
As you can see, identifying and managing hypermobile individuals can be a bit more time-consuming and challenging. Still, it can also be tremendously rewarding, as these folks are often chronically mismanaged by inattentive or unprepared trainers and therapists. This population is an outstanding opportunity to make a difference in someone’s life because of your unique expertise.
The Beighton Hypermobility Test is one of the screens we use in my new resource, The High-Performance Handbook, which is on sale at a great introductory price this week only. For more information