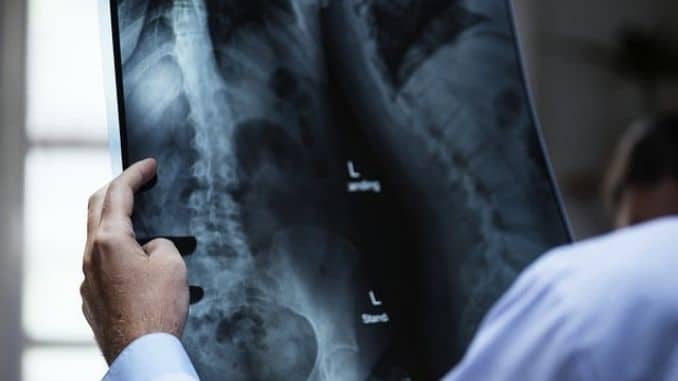
Don was worried that his active life was over. He’d just been diagnosed with spondylolysis, a defect in the spine that can cause low back pain, leg pain, and small stress fractures.
In a way, it was a relief — at least now he knew what was causing his pain. But he was also afraid of what it would mean. Did he have to stop running? Stop biking and hiking? Was he going to lose the things that he enjoyed in life?
Spondylolysis affects around 3 to 7 percent of Americans and is a common cause of low back pain in children and young people aged 26 and younger. It’s even more likely to affect teens and young adults participating in sports that place a lot of stress on the lower back or require hyperextensions of the spine, such as weightlifting, karate, soccer, football, and gymnastics.
Fortunately, it doesn’t mean your active life is over. Some treatments and exercises can help.
What Is Spondylolysis?
The spine has 33 bones called vertebrae. In between and to the back of these bones are “facet joints” that provide movement and help keep each vertebra in place. Fluid-filled discs exist between the bones as well, although more toward the front. They provide cushioning between the bones and keep movement flexible and easy while also stabilizing the spine.
Spondylolysis (pronounced spon-dee-low-lye-sis) is a condition that occurs when the pars interarticularis of the lumbar vertebrae suffers from a stress fracture ― either a crack or break.
The pars interarticularis, which means “part between the articulations,” exists between the facet joints. It is a small, thin bone that joins two vertebrae together. You can think of it like an isthmus — a narrow portion of land that joins two larger portions of land. In the same way, the pars interarticularis is a narrow piece of bone that joins two larger ones.
A fracture often occurs because of repeated stress on the spine. Imagine a metal coat hanger. If you bend it back and forth repeatedly, eventually it will break in the one area that you weakened with the repeated bending.
The same thing can happen to the spine if there is continued overload on the pars interarticularis without enough recovery time in between. Young people are most at risk for these injuries because their bones are still developing and haven’t reached their full strength. The vertebrae in the lower back are most commonly affected, although the condition can affect those in the neck as well.
Pars fractures usually occur on both sides of the vertebrae. Even if only one side is affected, however, the other then has to take on the full stress of the load and is likely to fracture soon after.
When the fracture occurs on both sides, that vertebra is no longer supported as it should be, and the spongy disc between the bones comes under additional stress. If the stress continues, the disc can start to stretch and may eventually tear and flatten out.
Without the disc to stop it, the vertebra above can start to slip forward onto the one below. If this occurs, it’s called “spondylolisthesis” ― in Latin, “oliothesis” means “to slip.” Spondylolysis may occur on its own or may develop together with spondylolisthesis.
What Are the Symptoms and Causes of Spondylolysis?
Sometimes, there are no symptoms that accompany this type of fracture. In other cases, people don’t develop symptoms until years later in adulthood.
When symptoms do occur, they typically include the following:
- Pain and stiffness in the back or neck that worsens with activity and improves with rest; the pain also worsens with hyperextension of the spine
- Pins and needles sensation in the legs
- Pain in the neck, legs, thighs or shoulders
- Headaches
- Muscle spasms or weakness
- Hamstring tightness, so that it’s difficult to bend forward
- Difficulty walking
- Posture changes, such as a backward pelvic tilt and stiff-legged gait
- Sciatica
Although the condition is most commonly caused by repeated stress, there are other potential causes as well:
- Birth defect
- Developmental problems early in life
- Arthritis
- Trauma, such as an acute fracture or injury
- Pathology, caused by cancer, infection or a benign tumor
- Postsurgical problems
Doctors usually use imaging tests to diagnose the condition, including lumbar X-rays, lateral X-rays, CT scans and MRIs.
How Are Spondylolysis and Spondylolisthesis Treated?
Treatment for these conditions always starts conservatively and depends on the severity of the pain and the slippage of the spine. Nearly all patients begin with the following:
- Rest — stopping sports activities
- Pain medications and muscle relaxants
- Chiropractic care
- Physical therapy
- Braces
If the pain persists, doctors may recommend other options like steroid injections and nerve root blocks. It’s only when all of these options fail that surgery becomes an option.
Most people have good luck healing a fracture with conservative treatments. About 80 to 85 percent of children and young people get better with time and care.
Sometimes, however, a pars fracture can be resistant to complete healing because of the following:
- It covers a small surface area
- The pars itself has little “spongy bone” inside to promote healing
- The area is constantly subject to motion and stress
The type of pars fracture can also make a difference in healing. Doctors typically classify them as follows:
- Atrophic fracture: The bone does not heal as it should. This is likely in a person with osteoporosis.
- Hypertrophic fracture: The ends of the fracture are thick, enlarged and next to each other, so they tend to heal well.
- Displaced fracture: The vertebra has slipped forward, so the ends of the fractured fragment are not near each other. This type doesn’t heal as well.
Depending on the type of fracture that’s present, healing may be delayed or may not proceed as expected. Fortunately, most people will feel better within three to six months, but it is important for them to rest and to avoid sports and strenuous activities during that time. If not allowed to heal properly, these conditions can lead to chronic back pain and loss of flexibility.
If all other treatments fail, surgery can be helpful. A fracture alone can be repaired with the use of a screw, which secures the two sides together and provides stability. If spondylolisthesis is present, spinal fusion may be necessary to fixes the bones in place. Both surgeries require between three and eight months of recovery before they become entirely stable.
Can Spondylolysis and Spondylolisthesis Be Prevented?
You can help lower the risk of these conditions with the following steps:
- Limit time spent on high-risk sports like diving, football, soccer, gymnastics, and wrestling
- Get adequate rest and recovery time between active times
- Warm-up properly before every game or practice
- Stretch regularly to keep muscles pliable and flexible
- Perform exercises to keep the core muscles strong, which help stabilize the spine
- Use safety equipment as directed
- Maintain a healthy weight
It’s also good to be aware of the risks and to understand the importance of taking care of the body. Pressure from peers, coaches, and parents can lead young people to push themselves too far.
7 Exercises That Help Heal Spondylolysis and Spondylolisthesis
Always check with your doctor first, then try the following exercises to help heal your spondylolysis or spondylolisthesis. Meanwhile, avoid potentially harmful exercises, including:
-
- High-impact exercises, including running, basketball, football, and others
- Heavy weightlifting
- Those that involve twisting or bending
CLICK HERE to watch the YouTube video.
1. Pelvic Tilt
Lie on the floor face up with your knees bent with your feet flat on the ground. Feel your spine lying flat against the ground underneath you. Flatten your back against the ground gradually, using your abdominal muscles to hold the position for about 15 seconds. Relax and repeat 10 times.
2. Double Knee to Chest
Lay face up on the ground with knees bent with your feet flat on the floor. Using your abdominal muscles, draw both knees up to the chest while keeping the spine flat on the floor. Hold for five to 10 seconds, then relax. Repeat 10 times.
3. Partial Curl
Start the same way, lying flat on the floor with knees bent. Tuck the chin and chest and curl the upper body only. Lift the shoulders off the floor while you extend your hands out in front of you. Do not lift any further but hold this pose for three to five seconds and then uncurl. Repeat 10 times for three sets.
4. Hip Roll
Lie down the same way as before with knees bent. Cross your arms across your chest and turn your head to the right. Let both knees fall slowly toward the left — the opposite direction — while continuing to look right. Hold for 10 seconds, then bring the knees back to the starting position and repeat on the other side. Repeat 10 times both sides.
5. Gluteal Stretch
Lie down on the floor in the same way with both knees bent. Rest the ankle of one leg against the knee of the other. Lace your fingers behind the thigh of the bottom leg and pull it toward your chest until you feel the stretch in the buttocks and outer portion of the hip. Hold for 15 to 30 seconds and then relax. Repeat on the other side for three repetitions each.
6. Hamstring Stretch
Sit on the ground with legs stretched straight out in front of you. Point your toes to the ceiling. Lean forward slowly, keeping your spine straight, until you feel the stretch in the backs of your legs (the hamstrings). Reach your hands forward and try to touch your toes. Hold for 30 seconds and relax, then repeat at least three times, trying to go a little farther forward each time.
7. Arm & Leg Raises
Start on your hands and knees. Raise one arm straight up in front of you, and then tighten the abdominals and raise the opposite leg straight out behind you. Hold for five to 10 seconds, then lower and repeat on the opposite side. Complete 10 repetitions on each side.
For your guide to eliminating lower back pain, make sure to check out Low Back Pain Solved, here!