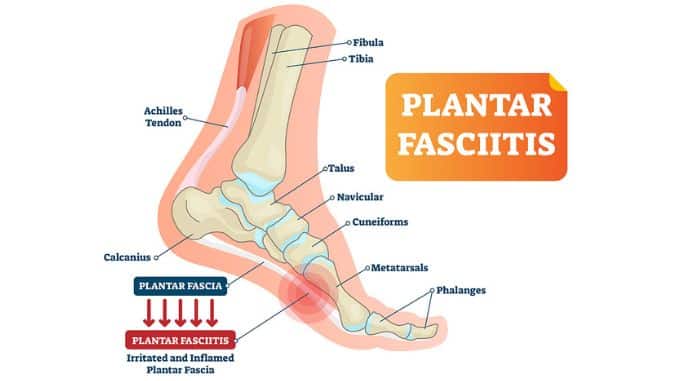
A lot of discomforts is likely when you have plantar fasciitis. You may have heard or read that this disease may be very unpleasant. On the other hand, how painful is it?
Because it’s so excruciating, many people with plantar fasciitis avoid going barefoot to alleviate their discomfort. Fortunately, there are some methods you may use to lessen the pain that comes with this problem.
In addition, some of these items are simple enough for everyone who suffers from it. Continue reading to learn more about this issue, the symptoms it might bring, and how to cope with the discomfort it may cause you.
How common is plantar fasciitis, and what makes you more likely to get it?
Plantar fasciitis affects about two million people in the United States yearly (Singh, Silverberg & Milne, 2009). The most frequent symptom of plantar fasciitis is discomfort in the soles of the feet. Injuries to the feet are prevalent among sportsmen (Singh, Silverberg & Milne, 2009). Professional athletes are more likely to suffer from plantar fasciitis if they engage in activities requiring weight on the ball of their foot. Other dangerous sports include road or track running, tennis, etc.
Ten percent of Americans suffer from plantar heel discomfort (Crawford, Atkins, & Edwards, 2000). It’s not only athletes that feel it. There was an unadjusted incidence rate of plantar fasciitis of 10.5 per 1000 person-years in the United States military (Scherer al. l, 2009).
People in their 40s to 60s are more likely to suffer from plantar fasciitis. Compared to males, women are twice as likely to experience this discomfort. Runners under the age of 20 are more at risk, as is anybody running in a group.
Plantar fasciitis is often the result of overuse and overcorrection in the gym. High-impact aerobic workouts, such as barefoot walking, lengthy periods of inactivity, and obesity, are among the contributing causes. Other activities that cause plantar fascia degeneration include plyometrics (athletic leaping), speed exercises, and graded hill runs. Running on unpadded or inadequately padded surfaces and wearing shoes with limited cushioning are well-known risk factors for Achilles tendon injuries. They might put a lot of strain on the heel while doing physical exercise.
What is the Plantar Fasciitis Stages?
PLANTAR FASCIITIS IN ITS EARLY STAGES
They may first notice a tingling sensation at the base of their heel. It may feel tight in the arch or sole because of a pull in the plantar fascia. Afternoons or after being weight-bearing for an extended period might bring on a sense of unease.
Plantar fasciitis should be treated or intervened in as early as possible to prevent the onset of a more chronic form of heel pain. It is valid for some individuals, but persistent plantar fasciitis and severe heel pain may develop in others. As a result, many patients fail to notice the early signs, believing their heel pain or stiffness will disappear.
Sports podiatrists often receive complaints about the sensation of a pebble or stone bruise in the shoe at this early stage. Patients with mild plantar fasciitis feel like they have stepped on gravel or a tiny stone. Plantar fasciitis does not always cause heel discomfort throughout the day in the early phases. It’s possible that the symptoms only appear in the morning when you first get out of bed. Some people experience discomfort again after a few days of being symptom-free.
Plantar fasciitis may cause heel discomfort as the foot touches the ground in the morning. However, this tends to be moderate and is frequently little more than a tingling sensation.
PLANTAR FASCIITIS – CHRONIC
Plantar Fasciitis symptoms get more severe when the ailment has progressed to a more advanced stage. If the tension on the plantar fascia continues for an extended period without being addressed, the issue will become chronic.
Patients who suffer from heel pain describe it daily, not only when they first get out of bed in the morning. Patients with plantar fasciitis stumble for at least five minutes after getting out of bed because of severe heel discomfort. A hot shower frequently alleviates heel discomfort within 15 minutes, and patients report feeling better afterward. As the plantar fascia inflammatory alteration is less constant and heel discomfort isn’t always present, walking throughout the day doesn’t always pose an issue.
Patients with Plantar Fasciitis get out of their automobiles after a long day at work and may experience discomfort. They feel better for the first few minutes, but only after a short distance. However, after a few thousand steps, the feet fatigue, and the heel discomfort returns in the afternoon.
Patients often tell their podiatrists that they hobble when they rise from a chair after supper or from a sofa while watching TV. The thickening of the plantar fascia owing to inflammation may be seen on an ultrasound.
SEVERE PLANTAR FASCIITIS
Plantar fasciitis may be severe or acute if pain develops suddenly, following a one-time occurrence, or on a specific day or activity. When persistent plantar fasciitis is ignored, it might progress to the same condition. The repeated strain on the plantar fascia has caused acute inflammation and severe discomfort. Extreme discomfort that lasts most of the day is common among patients with painful plantar fasciitis. These folks often use “excruciating” and “relentless.” Patients with chronic and acute diseases may experience throbbing when they sit or lie down and begin to feel the psychological implications. Those who have quit exercising and find it challenging to walk daily may suffer from plantar fasciitis.
X-rays are limited when dealing with plantar fasciitis, a soft tissue condition. Ultrasound scans, which we do as sports podiatrists, may assist in confirming or ruling out the damaged fascia.
Signs and Symptoms
The chronically strained or injured plantar fascia may cause acute, searing, or scorching foot pain by irritating the nerves that convey pain signals. It is possible to suffer from plantar fasciitis if you haven’t been able to walk for a lengthy period. In extreme cases, it is impossible to walk barefoot. Patients with plantar fasciitis find it challenging to get out of bed in the morning because of their pain.
The discomfort may be accompanied by a tingling feeling in more severe instances. Prolonged standing, walking, and applying physical pressure to the affected area exacerbate the pain. For example, heel raises, and toe walking (walking on tiptoes) might worsen the discomfort in the forefoot. In the windlass test, heel pain may be elicited by passive forefoot movement toward the body. As a result, it is a critical tool in diagnosing plantar fasciitis. An additional common sign is an antalgic posture, which includes walking or standing on the lateral border of the foot.
One foot is generally the only one affected by plantar fasciitis. It is more probable that bilateral symptoms will arise as a result of systemic arthritis.
How can I get rid of plantar fasciitis pain?
You may reduce plantar fasciitis discomfort in some ways. Reduce inflammation and discomfort by using over-the-counter pain medications. You may also find arch support and heel cups in specially made shoes. Stretching your plantar fascia might help avoid future damage and discomfort. Plantar fasciitis may be prevented and relieved with a few basic stretches, all of which can be found online. The towel stretch, for example, could be worth a go. Put a towel on the floor and place your forefoot on the towel to do this maneuver. Once you feel a little stretch in your forefoot from pulling your toes toward you, you’re done! If you can, hold this posture for at least 10 seconds before switching positions. The sitting forward bend is a yoga position that you may also practice. Sit on the floor with your legs bent at a 90-degree angle. When you feel a stretch in your heels, steadily bend forward with your hands on your knees until you feel it. Try to maintain this posture for a few seconds, and then repeat it a few times.
Conclusion
A very painful ailment, plantar fasciitis is one of the most common. Many methods are available to alleviate discomfort and avoid additional damage. Stretching, wearing specific shoes, and using over-the-counter pain medications are all options. No matter what you see in plantar fasciitis symptoms, consult a doctor.
Rick Kaselj, MS
Here are some other blog posts that may interest you:
If you like to learn more, then check out Plantar Fasciitis Relief in 7 days here: